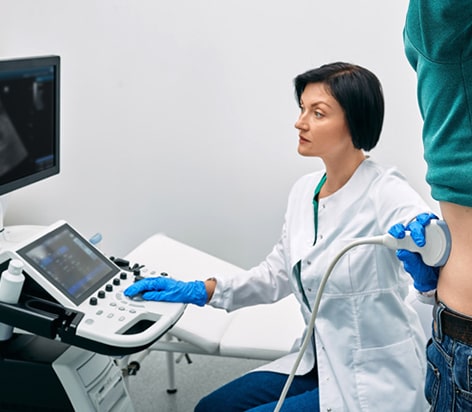
The renal critical care unit provides advanced treatment and care facilities for acute and chronic renal disease patients. The experts at the renal critical care unit have hands-on experience with the latest innovations related to renal replacement methods and delivering dialysis to critically ill patients. In addition, patients with severe fluid and electrolyte imbalances and acid-base disorders are also treated at the renal critical care unit.